Recent work supports the notion that the paraventricular nucleus (PVN) of the hypothalamus plays an important role in mediating increased sympathetic nerve activity during dehydration, hypertension, and heart failure. Little information is available about the types of PVN neurons involved in this sympathetic excitation or the properties of these neurons that are altered under these conditions. For many years, the paraventricular nucleus (PVN) of the hypothalamus has attracted attention as a supramedullary component of autonomic pathways mainly because of its role as an integrator of autonomic and neuroendocrine functions.
The PVN’s afferent and efferent connections make it easy to imagine it playing this role. There are direct projections from the PVN to autonomic sites including the rostral ventrolateral medulla oblongata (RVLM), the solitary tract nucleus, and the spinal intermedialateral nucleus (IML); and PVN neurons receive input from peripheral and central osmoreceptors, sodium receptors, and volume receptors.
What Is the Hypothalamus?
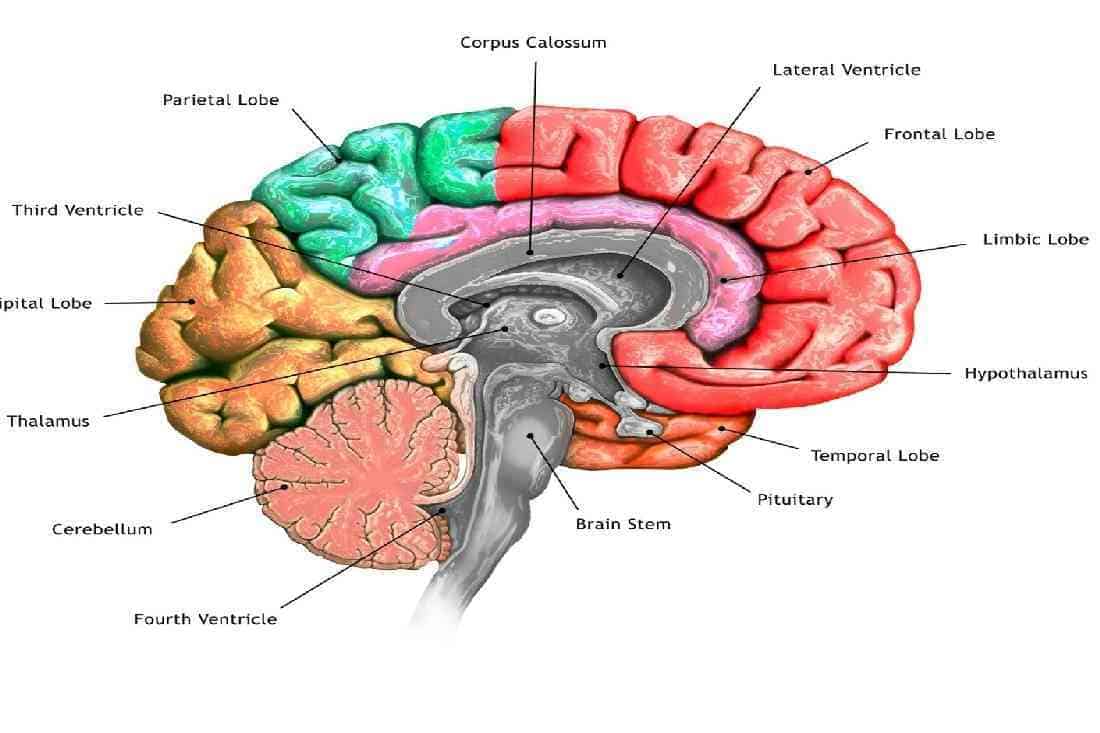
The hypothalamus takes up little space in the brain, but it houses important nuclei for many of the body’s regulatory functions. Located just below the thalamus, it keeps the body in homeostasis by controlling the sleep-wake cycle, body temperature, hunger and thirst, sexual desire, fluid balance, emotions, blood pressure, and heart rate.
The hypothalamus perfectly connects the nervous system with the endocrine system. As the body’s built-in alarm, it monitors and receives information from all parts of the body and then responds when necessary, by triggering the release of hormones by the pituitary gland.
Here are some additional facts about the hypothalamus:
- The hypothalamus makes up only 2% of the brain’s volume and is about the size of an almond.
- When the body experiences stress, the hypothalamus receives a distress signal from the amygdala and activates the sympathetic nervous system. The hypothalamus then sends signals to the adrenal glands to trigger the release of adrenaline into the bloodstream.
When danger is imminent, the hypothalamus helps keep the body on high alert by releasing corticotrophin-releasing hormone (CRH). CRH stimulates the pituitary gland to release adrenocorticotropic hormone, which causes the adrenal glands to release cortisol. This network between the hypothalamus, pituitary and adrenal glands is known as the HPA axis. A diet high in saturated fat can alter the way the hypothalamus regulates hunger and energy expenditure.
A healthy hypothalamus is supported by a diet rich in omega-3 foods (e.g. fish, walnuts, flaxseed and leafy greens) and vitamin-rich fruits and vegetables, vitamin C and B vitamins.It has been proven have shown that regular exercise improves hypothalamic regulation of the sleep-wake cycle, energy balance, and hormonal responses to stress.
The hypothalamus controls core body temperature through nerve endings in the skin and blood flow in the brain. When body temperature is too high, the hypothalamus causes blood vessels to dilate, which releases heat from the skin and increases the rate of sweating. When body temperature is too low, the hypothalamus conserves heat by initiating blood vessel contraction; it also generates heat by causing chills in the body.
Believe the Hype About the Hypothalamus
It’s an important part of how the endocrine system connects to your nervous system and plays a role in regulating bodily functions on many levels. It takes care of some of the day-to-day functions that you take for granted and don’t even believe is the part of your brain that does the thinking for you.
Here are some examples of what the hypothalamus regulates:
- Your appetite tells you when you’re hungry
- Thirst tells you when you need fluids
- When it’s time to sleep, when sleep is over
- Your body temperature
- Blood pressure
- Sexual arousal and general mood
Very important things about something the size of an almond. It’s located just below the thalamus, just above the brainstem. It controls metabolic processes and synthesizes and secretes neurohormones. These hormones control and regulate the secretion of pituitary hormones that connect the nervous and endocrine systems.
Hence what happens when the hypothalamus stops working properly? They may experience headaches, blurred vision, constant cold sensations, constipation, fatigue, weight gain, dizziness, or sexual weakness or dysfunction.
A lack of antidiuretic hormone production by the hypothalamus can also cause diabetes insipidus. This condition occurs when the kidneys cannot absorb water and the body cannot regulate how it uses fluids. Your doctor can run tests based on your symptoms that can determine the levels of your hormones, such as cortisol, estrogenic, growth hormone, prolactin, and testosterone. Your thyroid can be examined, and hypothalamic dysfunction assessed for precise treatments. Most causes of hypothalamic dysfunction are treatable, and the missing hormones can be replaced.
Hypothalamic Hormones
The hypothalamus is responsible for the production or control of many hormones in the body to maintain homeostasis. The hypothalamus works in conjunction with the pituitary gland, which produces and sends other important hormones throughout the body.
Together, the hypothalamus and pituitary gland control many of the body’s hormone-producing glands, called the endocrine system. These include the adrenal cortex, the gonads, and the thyroid.
Hormones secreted by the hypothalamus include:
- Antidiuretic hormone, which increases the amount of water the kidneys absorb into the blood
- Corticotrophin-releasing hormone, which helps regulate metabolism and the immune response by interacting with the pituitary and pituitary glands the adrenal gland works to release certain steroids
- Gonadotropin-releasing hormone, which tells the pituitary gland to release more hormones that keep the sex organs functioning
- Oxytocin, a hormone involved in several processes including the release of breast milk, moderating body temperature and regulating the sleep cycle
- Hormones that control prolactin, which tells the pituitary gland in nursing mothers to start or stop milk production growth
The hypothalamus also directly affects growth hormones. It tells the pituitary gland to increase or decrease its presence in the body, which is essential for both growing children and grown adults.
Disorders
A hypothalamic disorder is any disorder that prevents the hypothalamus from functioning properly. These diseases are very difficult to recognize and diagnose because the hypothalamus has multiple functions in the endocrine system.
The hypothalamus also serves the vital purpose of signalling that the pituitary gland should release hormones to the rest of the endocrine system. It is difficult for doctors to diagnose a specific malfunctioning gland, these disorders are often referred to as hypothalamic-pituitary disorders.
In these cases, there are some hormonal tests that doctors may prescribe to get to the bottom of the disorder.
Causes and Risk Factors
The most common causes of hypothalamic disease are head injuries affecting the hypothalamus. Surgery, radiation, and tumours can also cause diseases in the hypothalamus.
Some hypothalamic disorders have a genetic link to hypothalamic disorder. For example, in children, Kallman syndrome causes hypothalamic problems, particularly delayed or absent puberty, accompanied by an altered sense of smell.
Problems with the hypothalamus also appear to have a genetic link to Prader Willi syndrome. This is a condition in which a missing chromosome leads to short stature and hypothalamic dysfunction.
Additional causes of hypothalamic disorders may include:
- Eating Disorders, Such as Bulimia or Anorexia
- Genetic Disorders That Cause Excessive Accumulation of Iron in The Body
- Malnutrition
- Infections
- Excessive Bleeding
Symptoms of Hypothalamic Disorders
The symptoms of hypothalamic disorders vary depending on which hormones are in short supply. Boys may show signs of abnormal growth and abnormal puberty. Adults can show symptoms related to the various hormones that their bodies cannot produce.
There is usually a reasonable correlation between the lack of hormones and the symptoms they produce in the body. Symptoms of the tumour can include blurred vision, vision loss, and headaches. Low adrenal function can cause symptoms such as weakness and dizziness.
Symptoms caused by an overactive thyroid include:
- Sensitivity To Heat
- Anxiety
- Irritability
- Mood Swings
- Fatigue And Trouble Sleeping
- Lack Of Sexual Desire
- Diarrhoea
- Constant Thirst
- Itching
Diet Tips for Hypothalamic Health
Because the hypothalamus plays such an important role in the body, it is very important to keep it healthy. Although a person cannot completely avoid genetic factors, they can take nutritional steps to achieve ideal hypothalamic health daily to reduce the risk of hypothalamic disease.
The hypothalamus controls appetite, and foods in the diet affect the hypothalamus. Many studies have shown that a diet high in saturated fat can alter the way the hypothalamus regulates hunger and energy expenditure. Sources of saturated fat include lard, meat, and dairy products. Research has also shown that a diet high in saturated fat can have an inflammatory effect on the body.
This can cause the immune system to become overactive, making it more likely to target healthy cells in the body, increasing inflammation in the gut, and disrupting the body’s natural functioning.
Diets high in polyunsaturated fats, such as omega-3 fatty acids, can help reverse this inflammation. These fats could be a safe alternative to other types of oils and fats. Foods high in omega-3 include fish, walnuts, flaxseed, and leafy greens. Other healthy food options to support the hypothalamus and better brain function include:
- Vitamin-Rich Fruits and Vegetables
- Vitamin C
- B Vitamins
A functioning hypothalamus is one of the most important parts of the body and it usually goes unnoticed until it is no longer functioning properly. Following these nutrition tips can help keep your hypothalamus happy and functioning well.
Hypothalamic Er-Associated Degradation Regulates Pomc Maturation, Nutrition, and Age-Related Obesity
Hypothalamic pro-opiomelanocortin (POMC) neurons critically mediate leptin signalling and regulate feeding behaviour and systemic metabolic homeostasis through the secretion of various bioactive neuropeptides derived from the precursor protein POMC. POMC-derived neuropeptides, including adrenocorticotropic hormone (ACTH), α/β-melanocyte-stimulating hormone (α/βMSH), and β-endorphin, are critical for energy homeostasis and both POMC-deficient rodent models and human patients with POMC show mutations invariably hyperphagia and pronounced obesity.
Some of these mutations would be expected to alter POMC folding and turnover in the ER; for example, an autosomal dominant POMC cysteine phenylalanine mutation at position 28 (POMCC28F) has been identified in people with early onset obesity. In addition, dietary obesity is also associated with accumulation of POMC in the ER of POMC neurons. Although post-Golgi endoproteolytic cleavage of POMC has been well studied, the pathway for POMC conformational maturation within the
ER remains uncharted, and the molecular factors regulating POMC export from the ER remain unclear. Quality control systems typically maintain homeostasis and proteostasis in the ER throughout the lifespan of an organism. Disruption of ER homeostasis is a hallmark of several pathologies, including metabolic disorders and neurodegenerative diseases.
Quality control systems in the ER consist mainly of unfolded protein response (UPR) and ER-associated degradation (ERAD). UPR recognizes misfolded proteins in the ER and coordinates responses to environmental stimuli and stress differently across cell and tissue types. In the hypothalamic region of the brain, increased UPR activity has been shown to potentiate dietary obesity and mice overexpressing Der Xbox-binding protein 1 (XBP1) UPR effector in POMC neurons is resistant to dietary obesity through cellular and non-cellular mechanisms.
When the UPR Ire1α sensor is deleted in POMC neurons, mice are prone to dietary obesity with reduced energy expenditure. However, another group reported that POMC neurospecificity mice are resistant to diet-induced obesity with increased energy expenditure. The basis for these conflicting results is unclear, but the existence of such controversy underscores the need to clarify the physiological role(s) of ER quality control systems in POMC neurons.
The other important ER quality control mechanism uses the ERAD system, which involves the E3 ligase hydroxymethylglutaryl reductase degradation protein (Hrd1) and its silencing enhancer cofactor Linlike Protein 1 (Sel1L). This complex (Sel1LHrd1) represents the most conserved branch of ERAD that recognizes and targets ER proteins for cytosolic proteasomal degradation via the ubiquitin proteosome system.
The cofactor Sel1L, a single-segment ER transmembrane protein, is required for the stability of Hrd1. Although the biochemical processes of ERAD have been extensively studied over the past 2 decades, we are only just beginning to recognize the physiological role of ERAD in vivo (28). Sel1L or Hrd1 germline loss is lethal to the embryo and leads to premature death when induced in adult mouse models. Further characterization of cell-type specific Sel1L and Hrd1KO mouse models has revealed the cell-type specific importance of Sel1LHrd1 ERAD in health and disease. For example, Sel1L-deficient mice exhibit lipodystrophy and hyperlipidemia in adipocytes due to retention of lipoprotein lipase (LPL) in the ER.
In addition, mice with Sel1L-ablated arginine vasopressin (AVP) neurons progressively develop polyuria and polydipsia, hallmarks of diabetes insipidus, due to a maturation defect of the AVP precursor proAVP in the ER. These studies not only indicate the physiological (pathological) importance of cell type specific ERAD in health and disease, but also underscore our limited understanding of the role of ERAD in physiology.